Most medicines can’t get through the blood-brain barrier (BBB), a highly selective membrane that separates the circulatory system from the fluid bathing the brain. Certain peptides in animal venoms, however, can navigate across it to inflict damage. Now, researchers are capitalizing on venomous sneak attacks by developing a strategy based on a bee-venom peptide, apamin, to deliver medications to the brain.
The researchers will present their work today at the 253rd National Meeting & Exposition of the American Chemical Society (ACS). ACS, the world’s largest scientific society, is holding the meeting here through Thursday. It features more than 14,000 presentations on a wide range of science topics.
“We thought that because the venoms of some animals are able to attack the central nervous system, they should be able to go through the blood-brain barrier and possibly shuttle drugs across it,” Ernest Giralt, Ph.D., says. Apamin is known to accumulate in the central nervous system of people who’ve been stung by bees.
But the idea of using the apamin peptide itself had some drawbacks. “We knew we could not use apamin directly because it’s toxic,” he says. “But the good news is that the origin of the toxicity is well-known. We thought we could probably modify apamin in such a way that the toxicity would be eliminated, but it would still keep its ability to act as a transporter.”
Apamin’s toxicity stems from its interactions with a potassium channel in neurons. A positively charged group in the apamin molecule mimics the potassium ion and blocks the potassium channel when it binds. To eliminate the toxicity, Giralt’s group at the Institute for Research in Biomedicine (IRB Barcelona, Spain) removed the positively charged chemical anchor that attaches apamin to the channel. Then, the researchers checked to make sure the molecule could still cross the BBB. “This modification made apamin much less toxic, and its ability to cross the BBB was intact,” Giralt says. “This was very good news.”
As a next step, the researchers started tinkering with the molecule to make it smaller and also to make it invisible to the immune system to reduce potential side effects. Several versions of apamin later, they ended up with a promising version called Mini-Ap4. “It surprised us that this molecule crossed the blood-brain barrier much better than apamin itself — it was pure serendipity,” Giralt says. Mini-Ap4 also did not trigger a strong immune system response in animal models, an important factor in drug design.
Other BBB shuttles are in development, but many of them are based on linear peptides, which can be degraded by proteases before a medicine makes it to the brain. “Our niche is that our peptides are cyclic, or in a ring structure, making them completely resistant to proteases,” Giralt explains.
After these initial studies, the team will then put Mini-Ap4 to work, testing two different shuttling strategies. The first will be to simply attach Mini-Ap4 to a protein with a chemical bond and see if it can carry the cargo across the BBB. The second approach will involve filling a nanoparticle with medication and coating the nanoparticle with a forest of Mini-Ap4 molecules to facilitate the transfer across the BBB. The researchers will investigate these strategies in human cells and in mice.
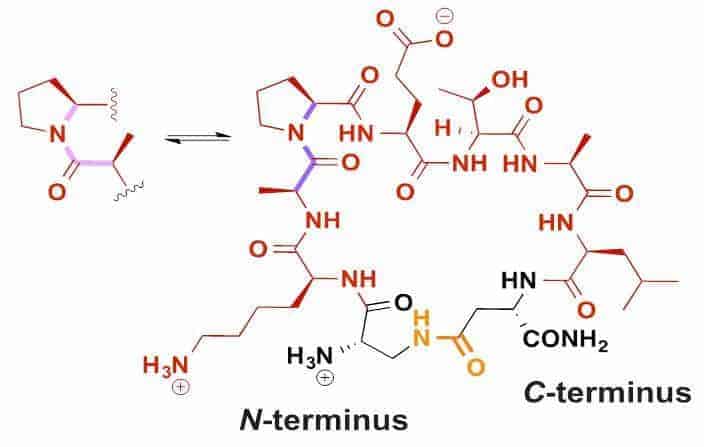
In other preliminary work, the researchers discovered that their version of apamin actually has two conformations, or shapes, and the team is using nuclear magnetic resonance spectroscopy to figure out which one is biologically active. “With that knowledge, we could design even better analogs,” Giralt says. He adds that a person who is allergic to bees probably wouldn’t be allergic to Mini-Ap4, but more work is needed to fully address this issue.