While fertility treatments have helped many people become parents, they commonly result in multiple births, increasing the risk of prematurity, and leading to lifelong complications. But this doesn’t have to be the case, according to Yale School of Medicine researchers and their colleagues, who recommend sweeping changes to policy and clinical practice in a study published in the April issue of Fertility & Sterility.
Pasquale Patrizio, M.D., professor in the Department of Obstetrics, Gynecology & Reproductive Sciences at Yale School of Medicine, and his colleagues at the Hastings Center identified several changes in policy and practice that can reduce the odds of multiple births and prematurity, expand insurance coverage for in vitro fertilization (IVF), and improve doctor-patient communications about the risks associated with twins.
IVF can cost upwards of $10,000 for a full cycle. Because few Americans have sufficient insurance coverage for fertility treatments, some patients feel financially compelled to maximize their pregnancy chances by implanting multiple embryos, despite the health risks and long-term costs associated with multiple gestations and births.
“Failure to cover these services causes harm to patients in addition to leading to multiple births,” said Patrizio. “When patients are better informed of the risks of multiples, and relieved of the financial pressures, research shows that they are more likely to choose to transfer one embryo at a time.”
Patrizio and his colleagues developed their recommendations through a research project that for the first time brought together fertility experts, representatives from the insurance industry and professional associations, and bioethicists. At a workshop, the group examined the causes and consequences of multiple births after fertility treatments.
Patrizio said the most promising changes should include: expanding insurance coverage to reduce the financial pressure on patients to prioritize pregnancy chances over safety; altering the definition of an IVF cycle so that two consecutive single embryo transfers is equivalent to one double embryo transfer for the purposes of calculating success rates and insurance benefits; investing in research to improve treatment efficacy and safety; fully informing patients of the likelihood of, and risks associated with, multiples; and altering clinic, insurer, and state policies to better enable patients to choose low-risk protocols.
“These policies have already been instituted in some European countries, and have resulted in a dramatic reduction in the rates of multiple births after IVF, while maintaining good live-birth rates,” said Patrizio.

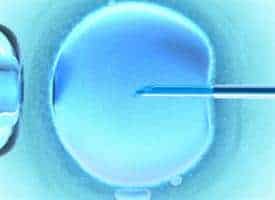
After reading this post I was in a bit of a catch. Of coarse people would consider IVF when they are struggling to conceive. But with all the risks it posed I would not recommend it.
As I understand , IVF isn’t exactly a pleasure. One would have to undergo hormone therapy to make sure that multiple eggs would mature. These would then be removed, inseminated outside the body (“in vitro”) with sperm, and implanted into a females body again. Some couples aren’t as lucky as others and don’t get a success with the first try. Although it may not matter in terms of looks, biological age does also matter when it comes to childbearing. And not to sound stereotypical, but at a young a couple is still climbing the career ladder, and funding can sometimes be a problem. The risks increases of stillbirth, neonatal death and disability in a new born child and of coarse down syndrome.
I personally think that the risk for IVF should be greatly considered. Accept for people having a lack of funding. How would one take care of the children if every single inseminated egg was successful?
But if this is promising it could be a revelation IVF. Of coarse the risk factor isn’t completely eliminated but at least the risk is fewer, but of coarse one could preach as much as one wants. When the clock is ticking and people want to start a family no risk will seem that big. The decision to have children is always completely personal.
I feel like reducing the possibility of multiple births when using IVF this will be extremely advantages as IVF always seemed like a catch 22; you got to have a child, however due to the cost multiple embryos are inserted to increase the chances of falling pregnant. However this in turn could result in complications and giving birth prematurely.
Some of the complications of multiple births include an increased risk of stillbirth, neonatal death and disability in new born child. Furthermore it increases the risk of complications to the mother, such as a late miscarriage, high blood pressure and pre-eclampsia (a multi-system disorder experienced by a pregnant woman which is usually characterised by high blood pressure)
In addition giving birth to 3 children or more at the same time isn’t very practical.
The solutions put forward in the article above seems realistic as the financial cost of IVF is substantial and naturally makes a hopeful parent want to make sure that they will fall pregnant after parting with so much money. Even if it means they will have triplets or even quadruplets which is ultimately unsafe for both the mother and the foetuses. If Medical Aids cover more of this this cost I too think that this will allow parents to focus more on safety, and essentially what they want, instead of focussing on the fact that this is their only chance to fall pregnant and implant many embryos.
However the idea that a solution to multiple births as a result of IVF put forward was to fully inform patients of the treatment and complications that can arise from multiple births is worrying as this should be happening now. All parents considering IVF should be given an intricate and elaborate explanation of both the procedure, possible outcomes and complications of the procedure. The implication that it is something that should change implies that it has not been done in the past which is not only careless but unethical.
In addition the couple wanting to have a child might be so set on proceding with IVF that they dont pay the necessary attention to the risks in which case they should be made even more clear.
Freezing fertilised embryos for later use in order to reduce the number of births at one time seems like the perfect solution. However, because the chances of implantation of embryos that have been frozen is significantly lower than those that are allowed to implant immediately is a large negative aspect to taking that route, and as a result hopeful couples choose not to take it and choose to risk multiple births instead.
Furthermore, as stated above, the problem with implanting fewer embryos and freezing others decreases the chance on implantation as well as giving birth to the strongest embryo that is most likely to survive as you are simply diminishing the chances of a healthy live birth as it is directly related to the the number of embryos allowed to attempt to implant.
Is there not another way to do this? Save some embryo’s for later use without diminishing their chances of implantation? So, in the end the chances of conceiving are not lowered as much when trying to prevent multiple births.
However, despite these flaws, with the average rate of multiple births when using VIF is 1 in 5, any measures taken to reduce this statistic should be incorporated thus diminishing the risks for couples who wish to conceive.
Well ; there are mathematical as well as medical reality flaws in the assumed cost/benefit analysis that will be gained as the end result of policy change .
The fundamental underlying reason that multiply embryo implantations ( rather than one or two ) are attempted during single IVF is : When these infertile women are stimulated with `ovulation ` hormone called FSH(Follucle stimulating Hormone) injections , the great majority of women respond with `Multiple follicle` formation in both ovaries as well as `Multiply ovulations` and chance of `retrieving of multiple (ovum)eggs` .
And the fact is fertilization of these retrieved multiple ovum are done immediately the ultrasonic retrieval of these eggs(ovum) with sperm to create multiple embryos . The dilemma has always been –Which embryo( s) has the best chance of success for a full term healthy baby – no method or test in this planet earth we live in can predict that for sure yet .
The ultimate chance of successful birth (whether you freeze the fertilized embryos for later implantation cycle or implant all of them does not change this fact at all . Low chance of successful birth after delayed implantation of frozen embryos ) in other words `You use all as you get them as soon as possible or you lose it ` reality surfaces very clearly .
Lets call a spade a spade here ; what is the fundamental motive for infertile couple in this very costly ordeal(both financially and emotionally) is to have a baby . Most couples do not care how many when fully informed about the realities and chances of successful outcome and the real statistical obstacles involved here ; without withholding any clinical success related real information and well known statistics , and frequently they (infertile couple) chose multiple implantations ( all they get in single FSH stimulation cycle ) rather than freezing some of them for `rainy day` later use . And of course IVF couple have every right to do so , you have to be honest with them for the real success statistics from the start on the medical ethical grounds as well as legally .
Successful outcome of healthy births at term delivery through IVF has so many `unknowable and unpredictable` factors involved . And unfortunately no one can predict the outcome one way or other , and you can not `design` a successful system that will reduce prematurity as well as cost involved for the insurance companies , IVF Centers or for the IVF couples involved . The factors for successful outcome are so many and incalculable . What ever method you chose or adopt will not change anything at the end . Insurance companies obviously in a bind and conflict with the IVF Centers and Infertile couple hopelessly stuck in between them . What and how many IVF procedures insurance companies are willing to pay has obvious limits of course , simply they can not cover this procedures indefinitely without a limit .
So the current practice is simply the practical result of –Cost and benefit(successful outcome of a birth or multiple births in a given cycle of attempt ) – rather than `Prematurity` or `low birth weight` due to multiple pregnancies and problem babies and children later years concerns – usually these has never been brought up as serious concerns in the infertility equation early on – simply this (multiply birth and prematurity and low birth weight ) are not the concerns – rather than` a baby` for the couple and these outcomes are not `predictable or preventable at all ` other than limiting the number of implantation in each cycle limits only the multiple births but NOT the prematurity or the low birth weight IVF babies . So we are talking to control if we can the `Multiple IVF pregnancy related prematurity and low birth weight babies here ` of course at the other end of the spectrum is obviously increasing the number of couples with `no babies for a given number of cycles attempted despite all the cost due to restricting the number of implantation in each cycle – a statistical fact – .
If you chose the `freeze` the embryos you get and limit the number of embryos you implant in each cycle you simply decrease the chance of live birth since the implantation chance as well as finding the best embryo out of bunch of available embryos as candidates to implant based on certain in perfect or perfect subjective `morphologic` characteristics of embryos and simply DOES NOT GUARANTEE success as normal birth – MOST IMPORTANTLY you can get premature as well as low birth weight birth DESPITE you had chosen to limit the number of implantations in each cycle …! You may simply end up implanting limited- 2 embryos at a time- indefinitely without a single successful outcome at all .. And the insurance companies has to pay the bill for more –unsuccessful cycles – as a result .
Punch line is : Multiple births and prematurities and low birth weight infants are all `expected` complications they are the results of Cost constrain as well as statistics and most importantly the medical realities of genetics ( variability of each and every individual as a men and a women )–fertilization- implantation- pregnancy physiology outcome- are all very closely interconnected and involved in incalculable and unknowable numerous factors .