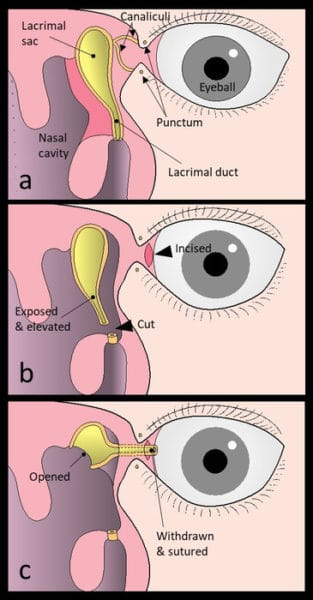
Under normal conditions, tears in the eyes are drained into the lacrimal sac through small openings called the upper and lower puncta located at the inner corner of the eye (called medial canthus). The tears go through small ducts called the superior and inferior canaliculi and then flow through the lacrimal sac and the nasolacrimal duct, and finally into the nose (Figure 1a). Obstruction in any part of the above-mentioned passage is the most common cause of watery eyes or epiphora. Epiphora affects the quality of life (QOL) of patients. When both the upper and lower canaliculi are obstructed, the tear fluid cannot be drained into the nose, resulting in epiphora. Although the cause of canalicular obstruction cannot be identified in many cases, it is thought to be associated with aging, trauma, tumors, and oral anticancer medication.
A minor surgery to enlarge the canaliculus by inserting a silicone tube is the common treatment to remove the obstructions. When the canaliculus is reoccluded or cannot be kept open, A Jones tube placement is considered, which semi-permanently places a glass tube that directly connects the nasal cavity and medical canthus. Otherwise, a surgery with an external incision may be considered, which leaves a scar of approximately 2 cm on the side of the nose.
To overcome the disadvantages of these conventional surgical methods, a team of otolaryngologists and ophthalmologists at Toho University Sakura Medical Center has developed a new procedure, ‘conjunctivoductivo-dacryocystorhinostomy.’
All surgical procedures are performed under general anesthesia. First, the entire lacrimal duct and lacrimal sac are exposed and elevated, and then the lacrimal duct is cut at the lower end (Fig 1b). At the medial canthus, the conjunctiva is incised (Fig 1b). The end of the cut lacrimal duct is withdrawn from the conjunctival incision and sutured to form a new lacrimal punctum (Fig 1c). Then the medial wall of the lacrimal sac is opened wide (Fig 1c). Now, the former lacrimal duct and lacrimal sac become the new lacrimal passage, and the tear fluid flows in this newly made passage.
The newly developed procedure, ‘conjunctivoductivo-dacryocystorhinostomy’ for the intractable canalicular obstruction does not leave any facial scarring or place foreign matter in the body. We believe that this procedure can help improve the QOL of patients with epiphora,” said Dr. Munetaka Ushio, lead author of the study. The study was published in The Laryngoscope on October 1, 2021.
Conjunctivoductivo-Dacryocystorhinostomy: A Novel Surgery for Intractable Canalicular Obstruction
Authors: Munetaka Ushio1, Hidetaka Masahara2, Masashi Sakamoto2, Yasushi Ohta1, Takatoshi Maeno2, Mitsuya Suzuki1
- Department of Otolaryngology, Toho University Sakura Medical Center
- Department of Ophthalmology, Toho University Sakura Medical Center
Media contact: Munetaka Ushio
Email: [email protected]
Telephone: +81-43-462-8811
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.