Researchers from The University of Texas at Austin and five other institutions have created a molecule that can cause cancer cells to self-destruct by ferrying sodium and chloride ions into the cancer cells.
These synthetic ion transporters, described this week in the journal Nature Chemistry, confirm a two-decades-old hypothesis that could point the way to new anticancer drugs while also benefiting patients with cystic fibrosis.
Synthetic ion transporters have been created before, but this is the first time researchers have shown them working in a real biological system where transported ions demonstrably cause cells to self-destruct.
Cells in the human body work hard to maintain a stable concentration of ions inside their cell membranes. Disruption of this delicate balance can trigger cells to go through apoptosis, known as programmed cell death, a mechanism the body uses to rid itself of damaged or dangerous cells.
One way of destroying cancer cells would be to trigger this innate self-destruct sequence by skewing the ion balance in cells. Unfortunately, when a cell becomes cancerous, it changes the way it transports ions across its cell membrane in a way that blocks apoptosis.
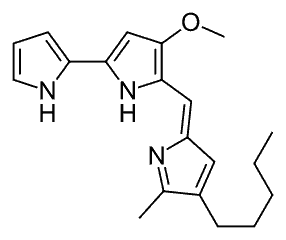
Almost two decades ago, a natural substance called prodigiosin was discovered that acted as a natural ion transporter and has an anticancer effect.
Since then, it has been a “chemist’s dream,” said Jonathan Sessler, professor in The University of Texas at Austin’s College of Natural Sciences and co-author of the study, to find “synthetic transporters that might be able to do exactly the same job, but better, and also work for treating diseases such as cystic fibrosis where chloride channels don’t work.”
Sessler and his collaborators, led by professors Injae Shin of Yonsei University and Philip A. Gale of the University of Southampton and King Abdulaziz University, were able to bring this dream to fruition.
The University of Texas members of the team created a synthetic ion transporter that binds to chloride ions. The molecule works by essentially surrounding the chloride ion in an organic blanket, allowing the ion to dissolve in the cell’s membrane, which is composed largely of lipids, or fats. The researchers found that the transporter tends to use the sodium channels that naturally occur in the cell’s membrane, bringing sodium ions along for the ride.
Gale and his team found that the ion transporters were effective in a model system using artificial lipid membranes.
Shin and his working group were then able to show that these molecules promote cell death in cultured human cancer cells. One of the key findings was that the cancer cell’s ion concentrations changed before apoptosis was triggered, rather than as a side effect of the cell’s death.
“We have thus closed the loop and shown that this mechanism of chloride influx into the cell by a synthetic transporter does indeed trigger apoptosis,” said Sessler. “This is exciting because it points the way towards a new approach to anticancer drug development.”
Sessler noted that right now, their synthetic molecule triggers programmed cell death in both cancerous and healthy cells. To be useful in treating cancer, a version of a chloride anion transporter will have to be developed that binds only to cancerous cells. This could be done by linking the transporter in question to a site-directing molecule, such as the texaphyrin molecules that Sessler’s lab has previously synthesized.
The results were a culmination of many years of work across three continents and six universities.
“We have demonstrated that this mechanism is viable, that this idea that’s been around for over two decades is scientifically valid, and that’s exciting,” said Sessler. “We were able to show sodium is really going in, chloride is really going in. There is now, I think, very little ambiguity as to the validity of this two-decades-old hypothesis.”
The next step for the researchers will be to take the synthetic ion transporters and test them in animal models.