Researchers at Washington University School of Medicine in St. Louis have discovered a promising new way to remove the harmful protein clumps that cause Alzheimer’s disease. By activating the brain’s immune cells, called microglia, with an antibody, they were able to reduce amyloid plaques and improve behavioral abnormalities in mice with Alzheimer’s-like disease.
Alzheimer’s disease starts with a sticky protein called amyloid beta that builds up into plaques in the brain, triggering a series of events that lead to brain shrinkage and cognitive decline. The new generation of Alzheimer’s drugs work by tagging amyloid for clearance by the brain’s immune cells. However, this new approach directly mobilizes the immune cells to consume the plaques.
“By activating microglia generally, our antibody can remove amyloid beta plaques in mice, and it could potentially clear other damaging proteins in other neurodegenerative diseases, including Parkinson’s disease,” explained the study’s senior author, Marco Colonna, MD, the Robert Rock Belliveau, MD, Professor of Pathology.
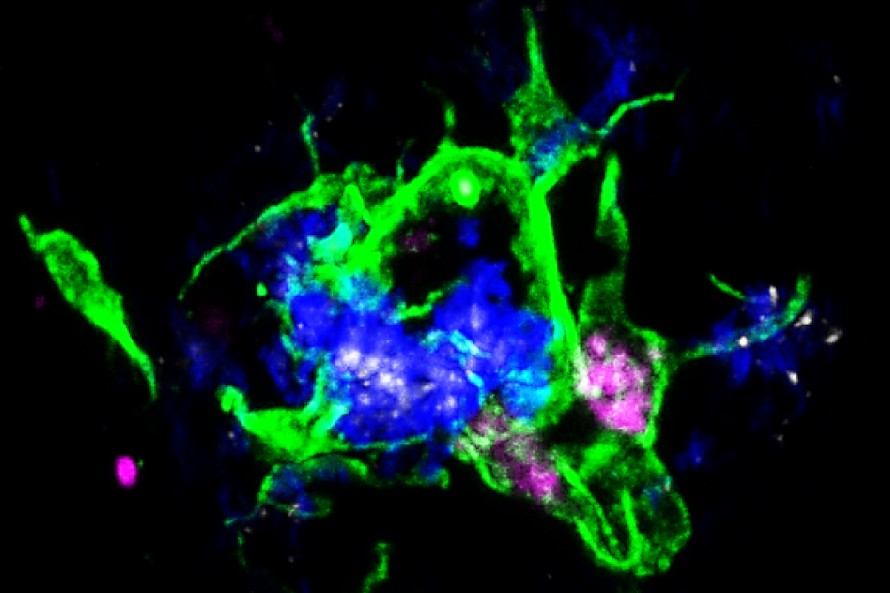
Microglia normally surround plaques to create a barrier that controls the damaging protein’s spread. They can also engulf and destroy the plaque proteins, but in Alzheimer’s disease, they usually do not. The researchers found that, in mice and people with Alzheimer’s disease, microglia that surround plaques produce a protein called LILRB4 on their cell surface, which inhibits their ability to control damaging plaque formation when it binds to another protein called APOE.
The researchers treated mice that had amyloid beta plaques in the brain with a homemade antibody that blocked APOE from binding to LILRB4. After confirming that the antibody reached the brain, they found that the activated microglia were able to engulf and clear the amyloid beta plaques. Clearing the plaques in mice also alleviated risk-taking behavior, which is a common problem in individuals with Alzheimer’s disease who may lack memory of past experiences to inform their decisions.
After amyloid beta plaques form in the brain, another brain protein called tau becomes tangled inside neurons. In this second stage of the disease, neurons die and cognitive symptoms arise. The researchers plan to test the antibody in mice with tau tangles to see if blocking the interaction between LILRB4 and APOE and activating microglia could alter later stages of the disease.
One potential side effect of drugs that target amyloid plaques directly is a condition called ARIA, which can cause swelling and bleeding in the brain when plaques are removed from brain blood vessels. The mice used in this study lacked amyloid plaques on blood vessels, so the researchers could not evaluate the risk of ARIA with this new approach. They are working with a different mouse model that does have plaques on brain arteries to understand if this new approach also carries a risk of ARIA.
“Lecanemab, as the first therapeutic antibody that has been able to modify the course of the disease, confirmed the importance of amyloid beta protein in Alzheimer’s disease progression,” said author David Holtzman, MD, the Barbara Burton and Reuben M. Morriss III Distinguished Professor of Neurology. “And it opened new opportunities for developing other immunotherapies that use different methods of removing damaging proteins from the brain.”
This new approach to treating Alzheimer’s disease by activating the brain’s immune cells to clear harmful protein clumps holds promise not only for Alzheimer’s but also for other neurodegenerative diseases that involve toxic protein buildup, such as Parkinson’s disease, ALS, and Huntington’s disease. Further research will be needed to evaluate the safety and effectiveness of this approach in humans, but these initial findings in mice are a promising step forward in the fight against Alzheimer’s and other devastating neurodegenerative diseases.