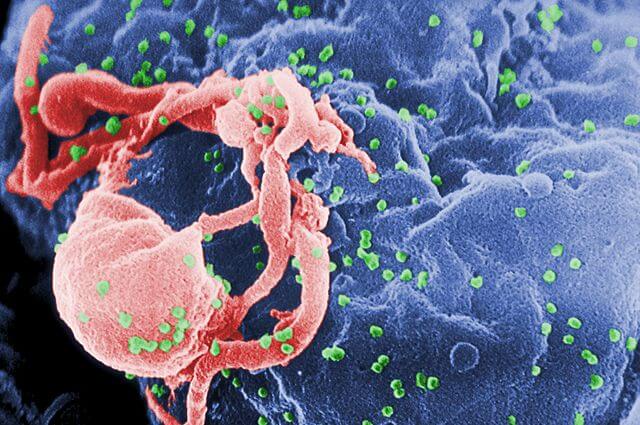
Infection by human immunodeficiency virus (HIV) causes acquired immunodeficiency syndrome (AIDS), a debilitating disorder in which progressive weakening of the immune system makes affected individuals more susceptible to potentially life-threatening infections and chronic diseases.
Despite advances in the treatment and management of AIDS, there is no cure, and HIV infection remains a major global health problem. According to the WHO, there were an estimated 34 million infected individuals in 2011. Over the last three decades, a number of animal models have been developed to study aspects of HIV infection, pathogenesis and control. However, the currently available models do not recapitulate the physiological environment of the most common route of HIV transmission worldwide, vaginal intercourse. Now, Mary Jane Potash and colleagues from St. Luke’s-Roosevelt Hospital Center and Columbia University Medical Center in New York, NY, have developed an approach for modelling heterosexual transmission of HIV in vivo. Their work was published recently in Disease Models & Mechanisms.
The work stems from an earlier collaboration between Potash and David J. Volsky (also from Columbia University); they established a chimeric HIV clone with a genetic modification that allows the virus to propagate in rodents instead of humans. Infection of mice with these viruses has been successfully applied to study aspects of HIV neuropathogenesis and to evaluate antiretroviral drugs and potential HIV vaccines. In their latest study, Potash and colleagues describe the efficient and reproducible transmission of chimeric HIV from infected male mice to uninfected females via mating, providing the first report of HIV transmission by coitus in an animal model. Treatment of females with antiretroviral drugs prior to mating prevented transmission of the virus, in line with observations in humans. Intriguingly, the efficiency of viral transmission declined during estrus in mice, providing evidence that the hormonal environment in the female reproductive tract can impact on host susceptibility to HIV infection. This finding has implications for HIV infection in humans, where it has been suggested that vulnerability to viral infection could vary during the menstrual cycle.
The model described here has several advantages compared with previous experimental approaches for investigating sexual transmission of HIV. For example, transmission occurs during mating, in contrast with earlier systems in which viral stocks need to be applied manually to the vaginal surface; thus, the system preserves features of the male and female reproductive tracts. This is important, as previous work has shown that host factors and cells in the seminal fluid activate cells in the female reproductive tract and enhance HIV infection, yet the underlying mechanisms remain poorly understood. Similarly, as indicated in this study, the local environment in the female reproductive tract can influence the rate and efficiency of HIV sexual transmission. By preserving the physiological features of coitus, the approach allows the dynamic aspects of viral sexual transmission to be investigated in vivo. Furthermore, the system can be used to investigate the efficacy of new interventive strategies aimed at preventing the most frequent route of HIV transmission.
“We developed this system to study HIV spread by mating in mice with the hope that it can be applied to promote practical approaches to prevent HIV sexual transmission to people at risk” explained Dr Potash, when asked about the goals of this research.