The warning arrives with an uncomfortable clarity, the kind that makes you sit up a little straighter. A new study from Cambridge and Glasgow shows that bird flu viruses can keep replicating even as the body heats itself into fever. The work, published in Science, identifies the viral gene that sets this dangerous resilience and explains why avian strains remain a major pandemic threat.
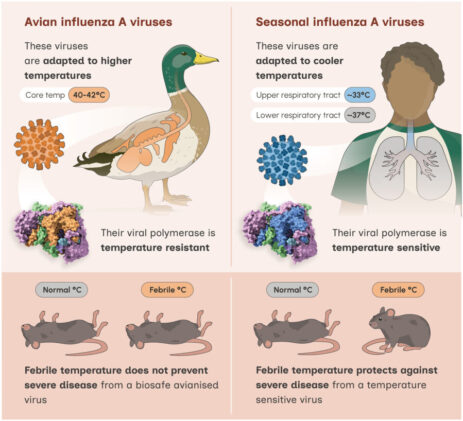
Seasonal influenza A viruses usually nestle into the cool upper airways, thriving at about 33C and slowing down as temperatures rise. Fever, one of the body’s oldest defense strategies, can push us toward 41C and often stops human flu viruses in their tracks. But avian influenza plays by different rules. Ducks, gulls, and other natural hosts run hot, often at 40 to 42C, and their viruses have evolved to be comfortable in that environment. The new research shows just how easily that comfort can spill over into human vulnerability.
The Gene That Lets Bird Flu Ignore the Heat
The team focused on a segment of the influenza genome called PB1, a component of the polymerase that drives viral replication. When this segment comes from an avian virus, the temperature sensitivity shifts. Replication continues even at fever levels, and the infection becomes difficult to contain. In the hyperthermic mouse model used in the study, a typical human-origin influenza strain collapsed under fever conditions while an avian-like PB1 version pushed forward and caused severe illness.
“The ability of viruses to swap genes is a continued source of threat for emerging flu viruses,” said Dr Matt Turnbull of the University of Glasgow. “We have seen it happen before during previous pandemics, such as in 1957 and 1968, where a human virus swapped its PB1 gene with that from an avian strain. This may help explain why these pandemics caused serious illness in people.”
It is a familiar, unsettling pattern. Influenza viruses can reassort their gene segments whenever two strains infect the same host. Pigs, which can be infected by both human and avian flu, act as informal mixing chambers. The study suggests that any future reassortment events involving an avian PB1 gene could give rise to a virus capable of thriving even as a human body fights back with heat.
In their in vivo work, the researchers mimicked fever by raising the ambient temperature around the mice. A simple two degree rise in body temperature, about what an everyday fever would produce, transformed a lethal human-origin infection into a mild one. The avianized mutant, however, barely paused.
The Surveillance Problem Everyone Saw Coming
That stubborn temperature resistance is exactly why avian spillovers continue to worry global health officials. H5N1, historically associated with a human mortality rate exceeding 40 percent, has been monitored for decades, and the new results only raise the stakes. If fever cannot slow a bird-adapted virus, early symptoms might offer far less protection than people assume.
“Understanding what makes bird flu viruses cause serious illness in humans is crucial for surveillance and pandemic preparedness efforts,” said Professor Sam Wilson of the University of Cambridge. “This is especially important because of the pandemic threat posed by avian H5N1 viruses.”
The implications stretch into clinical practice, too. Antipyretic drugs such as ibuprofen and aspirin are often used reflexively to reduce fever, though previous clinical evidence has suggested this may not always benefit the patient. The new findings underscore that fever itself, not only the immune response that accompanies it, can be directly antiviral. If a virus can tolerate those temperatures, the calculus of treatment shifts.
The study does not ask clinicians to change practice yet, but it does push researchers to rethink how temperature shapes viral evolution, human vulnerability, and the invisible negotiations between pathogen and host. It also reframes the surveillance challenge: the next dangerous strain may not be defined by its ability to spread quickly but by its ability to keep going when the body tries to shut it down.
For now, the focus turns to monitoring. Any avian influenza strain carrying PB1 gene signatures that support high temperature replication could signal a virus with pandemic potential. The work from Cambridge and Glasgow makes that possibility clearer than ever, and it adds new urgency to watching what birds shed, where it moves, and how easily it might fit inside a human body that is trying to burn the infection away.
Journal: Science
DOI: 10.1126/science.adq4691
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.