Every breath you take in a polluted city delivers something more than oxygen. Laced through the air are particles so fine they float for days, particles smaller than a bacterium that can travel deep into lung tissue, slip into the bloodstream, and, mounting evidence suggests, work their way through into the brain itself. Now, a study of almost 28 million older Americans has pushed that evidence further still, finding that long-term exposure to this fine particulate pollution raises the risk of Alzheimer’s disease through mechanisms that appear to act directly on the brain, bypassing the usual suspects of heart disease, high blood pressure, and depression.
The finding matters for a simple reason: Alzheimer’s disease has no cure. It affects around 57 million people worldwide, a number expected to triple by 2050, and the only real hope of stemming that tide lies in identifying risks we might actually do something about. Air quality, unlike age or genetics, is one of them.
The study, led by Yanling Deng at Emory University’s Rollins School of Public Health and published in PLOS Medicine, drew on Medicare claims data spanning nearly two decades. The researchers tracked who developed Alzheimer’s and what the air around their homes had contained in the preceding five years, carefully mapping concentrations of PM2.5, the fine particles at the centre of concern, to each participant’s zip code at one-kilometre resolution. Of the 27.8 million people in the cohort, roughly 3 million went on to develop Alzheimer’s. Each step up the pollution ladder, measured in increments of 3.8 micrograms per cubic metre of air, was associated with an 8.5 per cent increase in Alzheimer’s risk. That relationship held after accounting for dozens of variables, from income and education levels to smoking rates and body mass index across counties.
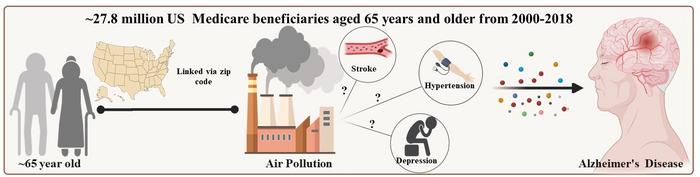
None of that will surprise researchers already tracking the PM2.5 and dementia literature. What the Emory team set out to resolve was a deeper question: how does pollution actually do this? The obvious candidates were the chronic diseases that trail dirty air wherever it settles, hypertension, stroke, and depression, conditions known to raise Alzheimer’s risk in their own right. If those were the primary pathway, cleaning up air would still help, but largely by preventing those intermediate conditions first.
The mediation analysis that Deng’s team ran told a different story. When they formally tested how much of the pollution-Alzheimer’s link ran through hypertension, stroke, or depression, the numbers were strikingly small. High blood pressure accounted for just 1.6 per cent of the association. Depression for 2.1 per cent. Stroke, the most vascular of the three, for 4.2 per cent. The remaining 90-odd per cent appeared to bypass these intermediaries entirely. As the authors put it, long-term exposure to fine particulate air pollution was associated with a higher risk of Alzheimer’s disease “largely through direct effects on the brain rather than through common chronic conditions such as hypertension, stroke, or depression.”
That phrase, direct effects on the brain, points towards mechanisms still being worked out but no longer entirely speculative. PM2.5 particles, and the inflammatory signals they carry, can cross the blood-brain barrier. Once inside, they appear to promote neuroinflammation and oxidative stress, and in children and young adults living in heavily polluted cities, post-mortem studies have already found the early protein deposits, amyloid-beta plaques, tau tangles, the hallmarks of Alzheimer’s, years or decades before they would be expected to appear. The implication is uncomfortable: pollution may begin setting the stage for dementia long before any symptoms surface.
One subset of participants showed a meaningfully different pattern. People who had already suffered a stroke carried a modestly but significantly elevated sensitivity to pollution’s effects on their Alzheimer’s risk. Where the broader population showed an 8.5 per cent increase per exposure increment, stroke survivors showed closer to 10.5 per cent. The Wald test confirmed the interaction was not a statistical fluke. The authors suggest the reason lies in what stroke does to the brain’s defences. A stroke can compromise the blood-brain barrier, the tight cellular seal that normally prevents large molecules and particles from entering neural tissue. With that barrier weakened, PM2.5 particles or their inflammatory messengers may penetrate more easily, worsening the neuroinflammation and amyloid accumulation that drive Alzheimer’s pathology. “Individuals with a history of stroke may be particularly vulnerable to the harmful effects of air pollution on brain health,” the authors write, calling it “an important intersection between environmental and vascular risk factors.”
The scale of the dataset provides a level of statistical confidence that smaller European studies, working with thousands rather than millions of participants, could not match. Earlier work from Swedish cohorts had suggested cardiovascular disease might mediate as much as half the pollution-Alzheimer’s association. But those estimates, as the Emory team note, were based on analyses that did not properly account for interactions between the pollution exposure and the mediating conditions themselves. When similar studies corrected for those interactions, their mediation estimates shrank dramatically, towards figures much closer to what this new analysis found.
Limitations remain. Pollution exposure was estimated at zip-code level rather than individual addresses, and indoor sources such as cooking and heating were not captured. The study population skews towards white, fee-for-service Medicare enrolees, so generalisability to other groups requires caution. And the five-year exposure window, though chosen deliberately, cannot capture what happened in participants’ lungs and brains across earlier decades of life.
But the policy logic the findings support is straightforward. Reducing ambient PM2.5 concentrations appears likely to reduce Alzheimer’s incidence through pathways that cardiovascular treatment alone cannot address. In a disease with no effective treatment, that may be among the most actionable levers available. For the one in five Americans who have survived a stroke, the implication is sharper still: the air outside their window is not a neutral backdrop, but something more actively working against the brain tissue they have left.
Study link: https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.1004912
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.

