The electrodes were already there. Surgeons had threaded them months earlier, fine wires snaking through millimetre holes in the skull to sit inside the brain itself, recording the electrical storms that define drug-resistant epilepsy. At a hospital affiliated with Southwest Jiaotong University in Chengdu, a team of neurosurgeons had been watching those storms, mapping where they started and how they spread, until they knew enough to act. Then they did something that the electrodes were not originally designed to do: they sent current down them in the other direction, heating a few millimetres of tissue to the point of destruction. The procedure is called radiofrequency thermocoagulation, and for years clinicians assumed it worked by burning out a small patch of misfiring brain. A new analysis suggests that assumption is wrong, or at least radically incomplete.
The finding matters because it reframes what minimally invasive epilepsy surgery actually is. Not a scalpel with better targeting. Something more like a system intervention, one that restructures how the whole network communicates.
When the Brain Won’t Stop Talking to Itself
Drug-resistant epilepsy is among the most disabling neurological conditions a person can live with. Around a third of the roughly 50 million people worldwide with epilepsy do not respond adequately to medication, and for them the options narrow quickly. Open resection surgery, which removes the seizure-generating tissue, works well when that tissue sits away from regions responsible for speech or movement. But when the epileptogenic zone overlaps with those critical areas, surgeons face an uncomfortable calculation: cut out the source of the seizures and risk the patient losing language, or leave it and watch the seizures continue. Radiofrequency thermocoagulation, guided by the same stereo-electroencephalography (SEEG) implants used for diagnostic monitoring, offers a third path. The electrodes create focal lesions a few millimetres across, small enough to be cautious, precisely placed, and made without any additional surgical opening of the skull.
What those lesions actually do to the wider brain, though, has been poorly understood. The working assumption was largely local: destroy the bad tissue, reduce the bad activity. Professor Haifeng Shu and Dr. Xin Chen at the General Hospital of Western Theater Command suspected the story was more complicated.
Their team studied 17 patients with medically refractory epilepsy, all of whom had undergone SEEG monitoring followed by RF-TC. The patients ranged widely in how bad things were: some had seizures daily, others monthly; the average person had been living with epilepsy for nine years before reaching this point. Crucially, the researchers analysed resting-state brain recordings taken immediately before the procedure and again immediately after its completion, measuring how different brain regions synchronised with each other across five frequency bands: delta, theta, alpha, beta, and gamma. This kind of functional connectivity analysis, borrowed from cognitive neuroscience, treats the brain not as a collection of discrete locations but as a network of nodes, linked by the degree to which their electrical activity rises and falls together.
Alpha Waves and the Architecture of Seizure
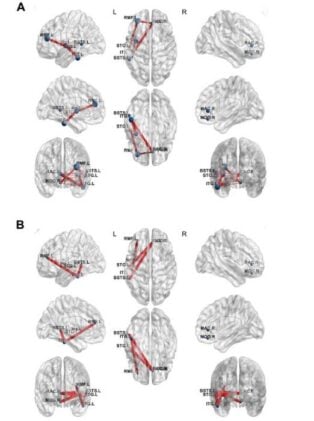
The clearest signal emerged in the alpha band, the roughly 8-14 Hz range classically associated with calm, wakeful brain states and what neuroscientists call thalamocortical gating, the brain’s mechanism for regulating which signals get amplified and which get filtered. After RF-TC, connectivity within the epileptogenic zone dropped significantly in alpha, and so did connectivity between the epileptogenic zone and the surrounding sampled regions. The seizure-generating tissue was not just quieter in its own neighbourhood; it was less tightly coupled to the rest of the network. When the team applied graph theory analysis, treating the connectivity data as a kind of map of the brain’s communication highways, they found that the betweenness centrality of nodes within the epileptogenic zone, roughly speaking how often those nodes sat on the shortest path between two other brain regions, also fell. The seizure-driving hubs were becoming less dominant in the network’s overall architecture.
“RF-TC appears to influence the epileptic brain as a network therapy rather than only a focal lesion,” said Prof. Shu. “Early electrophysiological signals after treatment may help clinicians understand whether the intervention is likely to be successful.”
That second sentence carries its own weight, because the team found something potentially useful wedged inside the data. Of the 17 patients, 10 showed meaningful clinical improvement after RF-TC, meaning at least a 50 percent reduction in seizure frequency or outright freedom from seizures. The remaining seven did not. And the patterns of connectivity change differed starkly between those two groups in ways that were measurable within minutes of the procedure ending. In patients who did not improve, alpha-band and theta-band connectivity dropped sharply and broadly, affecting both epileptogenic and non-epileptogenic brain regions. The researchers interpret this as maladaptive collapse: if the targeted lesioning failed to fully sequester the epileptic core, persistent pathological activity continued perturbing the wider architecture, dragging down synchrony in otherwise healthy regions. In patients who did improve, the picture was different. Their gamma-band clustering coefficient, a measure of local information processing and circuit organisation, actually increased after RF-TC. The brain, freed from the dominance of a pathological hub, appeared to reorganise locally in a more efficient direction.
The distinction is striking, but it comes with caveats. Seventeen patients is not a large cohort, and the study is retrospective. The analysis focused on short-term effects measured immediately post-procedure, not on how networks evolve over weeks or months. The team also did not separate out the propagation zone and irritative zone from the epileptogenic zone, which means some nuance about where exactly the network effects originate remains unresolved.
Rethinking What Minimally Invasive Surgery Actually Does
Still, the findings fit with a growing picture from other groups. A 2025 study by Gula and colleagues, using a different measurement technique involving direct electrical stimulation of the cortex, showed that RF-TC’s effects on brain connectivity extended up to 85 millimetres beyond the tiny ablation site, far further than any purely local explanation could account for. And work with virtual brain twin models, computational simulations of individual patients’ neural dynamics, increasingly supports the idea that focal interventions in epilepsy act by disrupting network hubs rather than simply destroying tissue. The thermocoagulation lesion, in this framing, is more like removing a key node from a complex graph than like excising a tumour. The rest of the network responds.
That reframing, if it holds up in larger studies, opens possibilities that are currently unavailable. If alpha-band connectivity immediately after RF-TC genuinely predicts whether a patient will respond, clinicians would have an early signal to act on, rather than waiting months to discover that the intervention wasn’t working. They could adjust: consider additional targeted lesions, shift to resection surgery sooner, or explore stimulation-based alternatives without the delay that currently complicates clinical decision-making. Dr. Chen described the team’s ambitions plainly: to combine brain-network analysis with individualized intervention planning so that each patient receives the most effective and least invasive treatment possible.
For now, those ambitions need larger prospective trials to test them properly. But there is something worth pausing on in the underlying idea. The electrodes that diagnosed the problem, mapped its extent, and revealed its network character are the same electrodes that, turned around, administered the treatment. And those same electrodes, recording in the quiet minutes after the heat dissipated, may already be telling clinicians whether the network they were trying to fix has actually started to change.
Read the study in the Chinese Neurosurgical Journal
Frequently Asked Questions
How is radiofrequency thermocoagulation different from regular epilepsy surgery?
Standard resection surgery physically removes a section of brain tissue, which can cause extensive disruption to the surrounding area and requires a significant craniotomy. RF-TC instead uses electrodes already implanted in the brain for diagnostic monitoring to deliver small, targeted bursts of heat that create lesions just a few millimetres across, without additional surgery. The new research suggests the treatment works not by destroying local tissue alone but by restructuring communication across the wider brain network, which may explain why its effects extend far beyond the tiny ablation site.
Why would a treatment that targets one small area change how the whole brain communicates?
The epileptic brain doesn’t just have a faulty patch; it has a faulty network, in which certain regions act as hubs that drive abnormal synchrony across distant areas. Removing or disrupting one of those hubs, even with a millimetre-scale lesion, can shift the entire network’s balance, similar to how removing a single major junction can restructure traffic patterns across a city. The Chengdu study found that connectivity between the epileptogenic zone and surrounding regions dropped significantly after RF-TC, and separate research has shown the procedure’s effects on brain signalling extend up to 85 millimetres from the actual lesion site.
Could doctors soon tell right after surgery whether the treatment worked?
That is exactly what this research is moving toward. The study found that the pattern of alpha-band brainwave connectivity recorded in the minutes immediately after RF-TC looked noticeably different in patients who went on to improve versus those who didn’t, suggesting those early signals could serve as a prognostic indicator. The limitation is that the finding comes from only 17 patients in a retrospective study, so it needs replication in larger, prospective trials before it becomes a reliable clinical tool.
Is RF-TC suitable for everyone with drug-resistant epilepsy?
No, and that’s precisely why its development matters. RF-TC is particularly valuable for patients whose seizure-generating tissue overlaps with regions responsible for language or movement, where conventional resection surgery carries too high a risk of permanent damage. It is a less invasive middle option, though current evidence suggests its seizure-control outcomes are generally somewhat lower than full resection for patients who are good resection candidates. Better ways to predict who will respond to RF-TC could help clinicians identify the patients for whom it is the right first step rather than a stopgap.
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.