THE MICE were nearly cancer-free. Twenty-six days after researchers injected them with aggressive colorectal cancer cells, cells engineered to spread to the lungs, the tumours had almost completely disappeared. Not shrunk. Not slowed. Vanished.
The treatment? Molecular clusters barely visible under a microscope, built from RNA and loaded with cancer-killing cargo.
Peixuan Guo at Ohio State University and his team have spent decades figuring out how to weaponize RNA’s versatility. The molecules can fold, twist and self-assemble like Lego blocks. They’re slippery enough to squeeze through tight spaces. And unlike many synthetic nanoparticles that accumulate in the liver or spleen, these RNA structures get rapidly cleared through the kidneys.
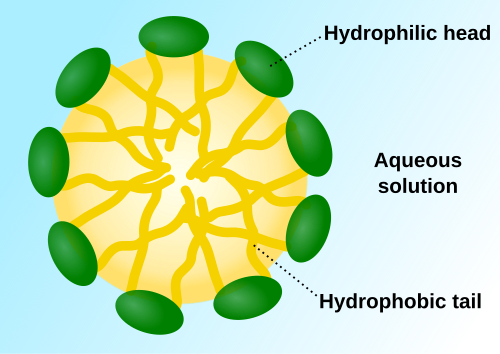
Now Guo’s group has packed those properties into what they call RNA micelles: spherical bundles of RNA strands that cluster around a cholesterol core. Each micelle carries ten copies of gemcitabine, a standard chemotherapy drug, along with small interfering RNA designed to shut down survivin, a protein that helps cancer cells resist death.
“It’s a two-pronged approach,” says Daniel Binzel, who worked on the study. The chemo damages DNA. The siRNA blocks the survival mechanisms cancer cells normally deploy in response. Attack from two angles simultaneously, and the cells can’t adapt fast enough.
What makes these micelles unusual is how they navigate the body. Their rubber-like flexibility lets them deform as they pass through leaky tumour blood vessels (a quirk of cancer biology that solid tumours create new, malformed vasculature). Once inside, a targeting molecule on the micelle’s surface latches onto EpCAM receptors overexpressed on colorectal cancer cells. The micelle binds, gets pulled inside, and releases its payload.
The team tested this in mice with a particularly nasty form of colorectal cancer: HT29 cells selected over multiple rounds of transplantation for their ability to colonize lungs. This model mimics human metastatic disease, where cancer spreads from the colon to the lungs. It’s a grim diagnosis. Only about 16% of patients survive five years.
Six injections over three weeks, starting five days after the cancer cells were introduced. Mice receiving micelles loaded with both gemcitabine and survivin siRNA were nearly tumour-free by day 26. Controls receiving either chemo alone or siRNA alone showed much less improvement. The combination was doing something neither therapy could manage independently.
There’s a broader context here. Small interfering RNAs have been hyped for cancer treatment since their discovery in 1998, but few have made it to approval. The problem has always been delivery. Getting siRNA where it needs to go without it being chewed up by enzymes or trapped in cellular compartments where it can’t function. And cancer cells are notoriously good at developing resistance to single therapies.
Guo’s team sidesteps both issues. The RNA structure itself provides protection and targeting. And by combining chemo with gene silencing in the same particle, resistance becomes harder. The cancer cell can’t just upregulate one pathway to survive.
“We showed that one nanoparticle can carry a drug and therapeutic RNA at the same time, and also used an RNA ligand,” Guo says. Three functions in one self-assembled structure: targeting, chemotherapy and gene silencing.
The micelles form spontaneously when you mix the right RNA strands in solution. Cholesterol tags on one strand drive assembly into spherical structures, much like soap molecules clump into bubbles. No complex manufacturing. No organic chemistry steps. Mix, heat, cool slowly. Done.
Guo’s enthusiasm is rooted in four decades of work. Back in the 1980s, as a graduate student, he published evidence that short segments of noncoding RNA had important cellular functions. A controversial claim at the time when RNA was viewed mainly as DNA’s messenger. His prediction that RNA therapeutics would become a major drug class has started to bear out, with recent FDA approvals for RNA-based treatments.
These mouse results need caveating, of course. Mice aren’t humans. Tumours grown from injected cell lines don’t perfectly replicate the complexity of cancers that develop naturally. And metastatic spread in mice happens faster and more predictably than the chaotic progression of human disease.
Still, colorectal cancer lung metastasis remains largely untreatable with current options, so even incremental progress matters. The researchers found no obvious toxicity from the micelles. No weight loss, no organ damage in preliminary safety checks. That’s not nothing. Chemotherapy’s side effects often come from hitting healthy tissue along with tumours.
The technology is already licensed to RNA Nanobiotics, a company in Cambridge, Massachusetts, which holds patents on Guo’s RNA nanoparticle platforms. Clinical trials would be the next step, though those timelines stretch years into the future.
The work also connects to a methodology paper the group published simultaneously in Nature Protocols, essentially a recipe book for building these structures. Other labs can now attempt variations—different drugs, different targeting molecules, different RNA configurations.
Kai Jin, the study’s first author and a PhD student in Guo’s lab, sees the micelle work as proof of concept for a broader idea. RNA’s modular nature means researchers can swap components in and out relatively easily. Want to target a different cancer? Change the surface ligand. Want to deliver a different drug? Modify the chemistry. The underlying scaffold remains the same.
Whether that modularity translates beyond mouse models remains to be seen. Human biology has a way of confounding even the most elegant laboratory demonstrations. But for now, those nearly tumour-free mice represent a small, tangible step forward for a disease that desperately needs one.
Study link: https://advanced.onlinelibrary.wiley.com/doi/10.1002/adfm.202521863
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.