A new surgical approach is rewriting the rules for brain and spine tumor care. Neurosurgeons at Beijing Tiantan Hospital have shown that combining embolization and resection in a single procedure can safely treat hypervascular central nervous system (CNS) tumors, which are among the most difficult lesions to remove.
The decade-long study, published in the Chinese Neurosurgical Journal, found that the one-stage hybrid operation reduced blood loss, improved patient outcomes, and avoided complications common in the traditional two-step process.
A longstanding neurosurgical challenge
Hypervascular CNS tumors, including meningiomas, hemangioblastomas, and paragangliomas, are riddled with dense blood vessel networks that blur boundaries and heighten the risk of massive bleeding during surgery. For decades, the standard strategy has been to first perform preoperative embolization, blocking key blood vessels feeding the tumor, and then return days later for resection. While widely used, this staged approach can trigger swelling, hemorrhage, and delays that put patients at greater risk.
In search of a safer alternative, Professor Yu Li, Professor Yi Lu, and their colleagues at Beijing Tiantan Hospital developed a workflow that integrates both treatments within a single surgical session. Conducted in a hybrid operating room equipped for both endovascular and open neurosurgery, the approach allows doctors to shift seamlessly from vessel embolization to tumor removal under one anesthesia.
How the one-stage hybrid operation works
- Selective embolization: Surgeons block deep or surgically inaccessible arterial feeders while leaving superficial vessels to be managed during resection.
- Flexible materials: They employ ethylene vinyl alcohol copolymer (EVOH), detachable coils, or silk suture fragments to occlude vessels, and balloon catheters when temporary control is needed.
- Immediate resection: With blood flow already reduced, the tumor is removed in the same session, minimizing the interval risks of swelling and hemorrhage.
This targeted strategy avoids complete devascularization, which can harden tumors and make them more difficult to remove. Instead, it reduces bleeding enough to make resection safer.
Results from a decade of cases
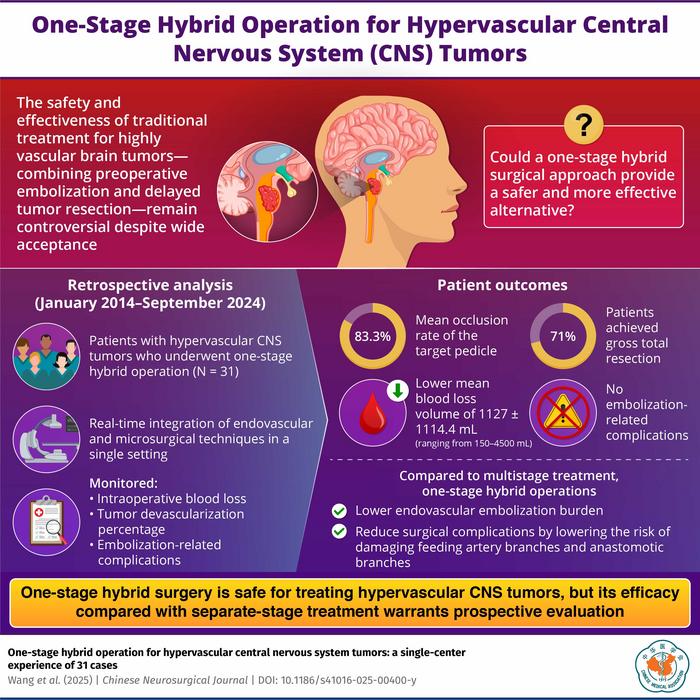
Between 2014 and 2024, the team treated 31 patients using the hybrid approach. Results were encouraging:
- Gross-total removal was achieved in 71 percent of cases.
- Near-total removal in 19.4 percent, and partial removal in 9.7 percent.
- Blood loss averaged more than one liter less than typically reported in staged procedures.
- Complications: None were linked to embolization.
- Recovery: At discharge, 87 percent of patients had stable or improved neurological function. At 12 months, two-thirds were symptom-free.
One case highlighted in the study involved a 73-year-old man with a large cerebellar hemangioblastoma. Using the hybrid method, surgeons successfully cut blood supply from inaccessible feeders and resected the tumor in one operation. He was discharged in 10 days, and follow-up imaging confirmed complete tumor removal.
“Our experience shows that the one-stage hybrid operation is both safe and effective for managing hypervascular CNS tumors,” said Professor Yi Lu, lead investigator of the study.
What this means for the future
The study demonstrates that a single-session procedure can address the risks of staged treatment while maintaining tumor control. By reducing blood loss, protecting neurological function, and avoiding embolization-related complications, the one-stage hybrid operation could mark a turning point in neurosurgery. However, the authors emphasize that their study was retrospective and relatively small in scale. Larger prospective trials will be necessary to confirm its superiority.
If validated, this method may become a new standard of care for hypervascular CNS tumors, offering patients safer and more efficient treatment in one sitting rather than two.
Journal: Chinese Neurosurgical Journal
DOI: 10.1186/s41016-025-00400-y
Discover more from SciChi
Subscribe to get the latest posts sent to your email.