A simple pulse through the skin may one day soothe stubborn stomach pain.
A new review in the Journal of Translational Gastroenterology finds that transcutaneous vagal nerve stimulation (tVNS), a non-invasive way of activating the vagus nerve, shows promising results for gastrointestinal disorders. Clinical trials suggest that tVNS can reduce abdominal pain, improve motility, and even calm gut inflammation in conditions such as irritable bowel syndrome (IBS), functional dyspepsia (FD), gastroparesis, and inflammatory bowel disease (IBD).
How the Vagus Nerve Shapes the Gut
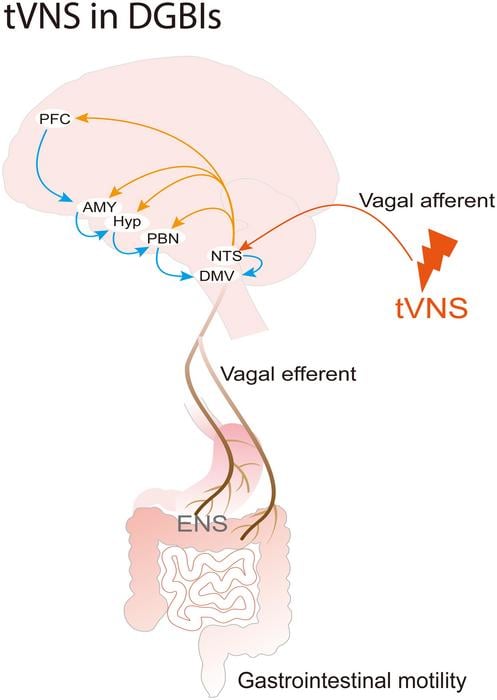
The vagus nerve, the body’s longest cranial nerve, connects brain and gut through a two-way flow of signals. It influences motility, satiety, secretion, and inflammation. When vagal activity dips and sympathetic tone dominates, the result can be abdominal pain, sluggish motility, or chronic gut inflammation. Traditional vagal stimulation requires surgical implants. tVNS, delivered through electrodes on the ear, neck, or skin, offers a far less invasive route.
Evidence From Clinical Trials
Trials reviewed by Jieyun Yin and colleagues show consistent, if preliminary, benefits:
- Functional dyspepsia: In a multicenter study of 330 patients, taVNS cut stomach pain rates by up to 82.8% compared to 61.5% for sham therapy.
- IBS-C: Patients saw a 64% drop in abdominal pain and tripled weekly bowel movements after 4 weeks of taVNS.
- Gastroparesis: An open trial of handheld cervical stimulation (gammaCore) improved nausea, fullness, and pain in 15 patients.
- Pediatric IBD: In a pilot of 22 children, 50% with Crohn’s disease and 33% with ulcerative colitis achieved remission after 16 weeks of taVNS.
- Adolescents with IBS: Percutaneous electrical nerve field stimulation (PENFS) delivered sustained pain reduction across randomized controlled trials.
Mechanisms at Work
The review points to overlapping pathways:
– Anti-nociceptive effects: tVNS dampens visceral hypersensitivity by modulating vagal afferent signals to brainstem centers.
– Anti-inflammatory effects: Acetylcholine released by vagal activity binds to α7 receptors on macrophages, suppressing TNF-α, IL-6, and IL-1β.
– Prokinetic effects: tVNS boosts gastric accommodation, esophageal sphincter tone, and rectoanal reflexes, supported by heart rate variability measures of parasympathetic activity.
“Transcutaneous VNS has been shown to relieve abdominal pain, improve GI symptoms, and accelerate GI motility by enhancing vagal activity in patients with various GI disorders.”
Limitations and Next Steps
Despite the encouraging data, most trials remain small and vary in frequency, duration, and stimulation site. Animal studies hint that higher-frequency stimulation may be optimal for pain, while lower frequencies may better support motility. Standardized protocols are needed, as are larger multicenter randomized controlled trials.
“Transcutaneous VNS appears to be an emerging, effective, low-cost, and safe therapy for GI disorders. However, in-depth research is needed to elucidate the mechanisms of action.”
Takeaway
Non-invasive vagal nerve stimulation shows potential to reduce pain, restore gut motility, and ease inflammation in conditions like IBS and IBD. While early results are strong, the field needs larger, standardized studies to confirm benefits and refine treatment protocols.
Key Findings
- tVNS reduced stomach pain in 330 functional dyspepsia patients, outperforming sham therapy.
- IBS-C patients experienced a 64% pain reduction and tripled bowel movements after taVNS.
- Pediatric IBD remission reached 50% for Crohn’s disease and 33% for ulcerative colitis after taVNS.
- Mechanisms include anti-inflammatory, anti-nociceptive, and prokinetic pathways tied to vagal activity.
The field is moving fast, with research expanding into personalized neuromodulation and brain-gut imaging. If confirmed, tVNS could offer patients a safe, accessible alternative to medications and surgeries for stubborn GI symptoms.
Journal: Journal of Translational Gastroenterology
DOI: 10.14218/JTG.2025.00024
Discover more from SciChi
Subscribe to get the latest posts sent to your email.