Millions of patients endure hours without food or water before surgery, following medical guidelines dating back to 1946.
But a comprehensive analysis of modern research finds no evidence that pre-surgical fasting actually prevents the dangerous complications it was designed to avoid, raising questions about whether this uncomfortable practice remains necessary.
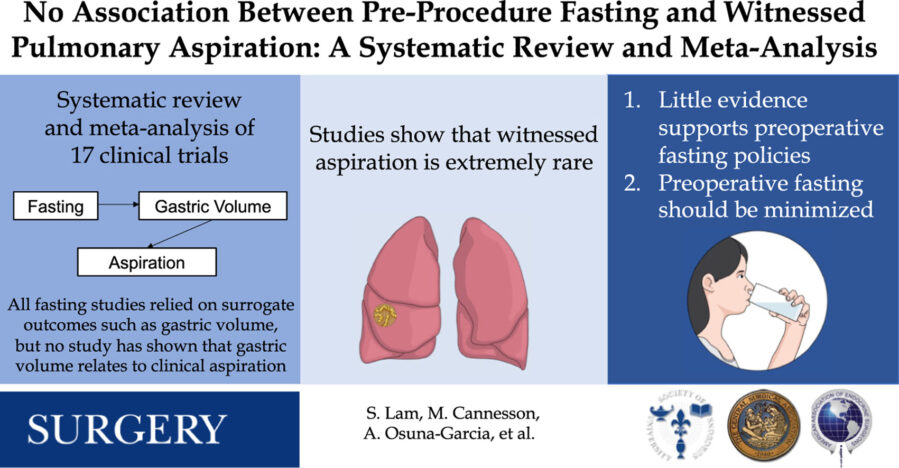
UCLA researchers analyzed 17 studies involving nearly 1,800 patients and discovered that fasting before surgery showed no association with preventing aspiration—the potentially deadly condition where vomit enters the lungs during anesthesia. The findings challenge one of medicine’s most universal pre-operative practices.
Questioning Medical Orthodoxy
The fasting requirement emerged nearly 80 years ago when doctors first identified a possible link between stomach contents and aspiration pneumonia. Since then, patients have routinely been told to avoid food and water for 8-12 hours before procedures, creating what many describe as one of surgery’s most dreaded aspects.
The UCLA team examined randomized clinical trials and observational studies published between 2016 and 2023, focusing specifically on witnessed aspiration events rather than indirect measures. What they found surprised them: aspiration occurred in just 4 of 801 patients who had more liberal fasting rules (0.50%) compared to 7 of 990 patients following traditional fasting protocols (0.71%).
The difference wasn’t just statistically insignificant—it actually favored the group that fasted less. The odds ratio for aspiration was 1.17, with a confidence interval spanning from 0.32 to 4.23, indicating no meaningful association between fasting duration and aspiration risk.
Key Research Findings
The study revealed several important patterns about surgical fasting:
- Aspiration events remained extremely rare regardless of fasting duration
- Most previous research relied on surrogate measures like stomach acid levels rather than actual aspiration
- Trial sequential analysis suggests future studies are unlikely to find different results
- Current hospital practices often extend fasting far beyond recommended guidelines
- Modern assessment methods like gastric ultrasound could replace blanket fasting rules
Perhaps most telling, the researchers discovered that previous studies focused on measuring gastric volume and pH levels—factors that have never been proven to correlate with actual aspiration in humans under anesthesia. This suggests decades of research may have been chasing the wrong endpoints.
The Human Cost of Caution
“At some point, almost everybody will undergo a procedure and there are universal policies in every healthcare facility that require some degree of fasting before surgery,” explained Dr. Edward Livingston, health sciences professor of surgery at the David Geffen School of Medicine at UCLA and the study’s senior author. “Fasting for long periods of time is extremely uncomfortable and patients really don’t like to do it.”
The researchers had already examined real-world fasting practices across more than 80 hospitals, finding that patients routinely fast much longer than guidelines recommend. This creates unnecessary suffering without apparent medical benefit.
The disconnect between guidelines and practice isn’t surprising. Operating room schedules change, procedures get delayed, and the easiest solution is often to keep patients fasting “just in case.” But if fasting doesn’t prevent aspiration, these extended periods of discomfort serve little purpose.
Looking Toward Personalized Approaches
Rather than abandoning precautions entirely, the research points toward more sophisticated risk assessment. Modern techniques like preoperative gastric ultrasound can directly visualize stomach contents, potentially allowing doctors to make individualized decisions about when surgery is safe.
This shift from universal rules to personalized medicine reflects broader trends in healthcare. Instead of applying one-size-fits-all policies, medical teams could assess each patient’s specific risk factors and stomach status immediately before surgery.
As medical practices evolve, this study suggests it may be time to reconsider traditions that cause patient discomfort without clear benefit. The next step involves prospective trials where fasting times are reduced while modern monitoring ensures patient safety—potentially ending decades of unnecessary hunger for surgical patients.
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.