Key Takeaways
- Researchers integrated curcumin and ginger extracts into titanium implants to enhance bone healing and combat infections.
- The innovative design addresses challenges faced by millions of patients with metal implants, where infection rates are significant.
- In animal tests, the combination greatly increased new bone formation and effectively killed bacteria, providing dual benefits.
- This approach aims to improve outcomes for various orthopedic implants, potentially extending to other conditions like arthritis.
- Future research will assess the long-term performance of these drug-loaded implants under human joint loading conditions.
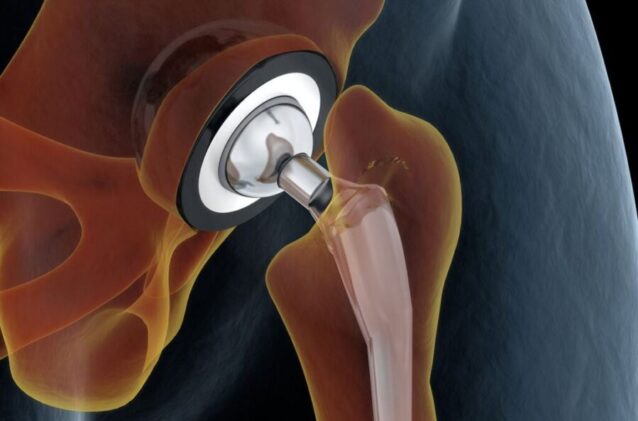
The titanium cylinder is about the width of a pencil, four millimetres tall, and milled to fit precisely into a drilled channel in living bone. Its surface, roughened at the microscopic scale, is sprayed with a calcium phosphate mineral that mimics the chemistry of the skeleton itself. And then, pressed into that ceramic layer, something rather unexpected: the active compounds from two kitchen spices that have been used in Indian and Chinese medicine for thousands of years. Researchers at Washington State University have loaded implants like this one with curcumin, the bright-yellow molecule responsible for turmeric’s colour and much of its reputed medicinal punch, alongside an extract of ginger root. In early animal tests, the combination roughly doubled the rate at which new bone locked around the implant, killed more than nine out of ten bacteria on its surface, and slashed the viability of bone cancer cells by a factor of eleven.
The problem these spice extracts are being asked to solve is not a small one. Around 7 million Americans are currently living with metal hip or knee replacements, and failure rates vary more than most patients realise: some designs of coated femoral stem show revision rates approaching 23% at 17 years, and roughly a third of implant failures involve bacterial infection of the metal surface itself.
Susmita Bose, the Westinghouse Distinguished Chair Professor in WSU’s School of Mechanical and Materials Engineering and the paper’s corresponding author, has spent years refining how implants bond with bone, building on earlier work in 3D-printed bone scaffold fabrication that was once considered speculative but is now fairly standard in orthopaedic manufacturing. Her interest in natural compounds grew partly from epidemiological observations: populations with high dietary curcumin consumption show lower rates of inflammatory bone loss, and ginger has documented effects on osteoclast activity (the cells that break bone down) and bone mineral density. The logic of loading those compounds directly onto an implant, rather than trying to deliver them systemically, is that the dose goes exactly where it’s needed and keeps releasing slowly over weeks rather than flooding the body all at once. “Basically, I say it’s combining the best with the latest,” Bose said. “The best part is from the food, and the latest aspect comes from the biomedical device.”
Bacterial infection of a metal implant is one of the hardest complications in orthopaedic medicine to treat, partly because bacteria form biofilms on metal surfaces that antibiotics struggle to penetrate, and partly because systemic drug delivery cannot concentrate enough medication at the implant site. In roughly a third of implant failure cases, infection is a contributing factor, and the standard solution, removing the implant entirely, is an ordeal with serious recovery implications. Approaches that build antibacterial properties directly into the implant surface are one of the more promising ways to reduce that risk.
Curcumin interferes with a molecular signalling pathway called NF-kB, which cancer cells rely on to avoid the programmed cell death that normally culls damaged or abnormal cells. By inhibiting the phosphorylation step that activates NF-kB, curcumin can arrest cancer cell proliferation and reduce tumour growth at the local site. In osteosarcoma, which is the most common bone cancer in children and adolescents, this targeted suppression is particularly relevant because the disease recurs locally even after surgery; a slow-releasing implant coating that continues to suppress residual cancer cells could potentially improve outcomes beyond what chemotherapy alone achieves.
Curcumin and ginger extract have long safety records as dietary compounds, and at the doses used in this study, neither showed toxicity to healthy bone-building cells (osteoblasts) in culture; in fact, osteoblast viability increased significantly in the presence of both compounds. The more relevant question for long-term clinical use is how the ceramic coating behaves mechanically over years of joint loading, since coating delamination is a known failure mode for hydroxyapatite-coated implants more broadly. That question will need to be answered in larger animal models and eventually human trials before the approach can be translated to clinical use.
The researchers suggest the platform is applicable to any load-bearing implant site, including hip, knee, spinal, and shoulder replacements, not just cases involving cancer. The antibacterial and bone-bonding benefits are relevant across all orthopaedic implantation, and the anti-inflammatory properties of curcumin could be useful in patients with conditions like rheumatoid arthritis, where inflammatory bone loss is an ongoing problem. The modular nature of the coating, where different active compounds could in principle be loaded onto the same hydroxyapatite carrier, opens the question of whether other natural or synthetic drugs could be incorporated in a similar way.
The implant design involves several layers working together. A titanium alloy core, Ti-6Al-4V, provides the structural backbone; it is strong, lightweight, and the body tolerates it reasonably well. That core is then plasma-sprayed with hydroxyapatite doped with zinc oxide, building a ceramic coating between 80 and 150 micrometres thick. Zinc is not incidental here.
Zinc ions promote osteoblast proliferation through a pathway involving the OPG/RANKL ratio (essentially, the molecular balance that tips cells toward building bone rather than resorbing it), and they kill bacteria through two distinct mechanisms: generating reactive oxygen species that breach bacterial cell walls, and binding selectively to transporters that bacteria rely on to absorb the nutrient manganese. Starved of manganese, the bacteria die. Curcumin and ginger extract then add their own polyphenolic chemistry to that antibacterial effect. The result, tested against Staphylococcus aureus, the species responsible for many of the nastiest implant infections, was approximately 92% bacterial kill. “Often, an infection will require the removal of the implant,” Bose noted. “There is no other way of fixing bone in patient’s body. So, infection-related problems can cause really a huge health issues and financial burden.”
The anti-cancer mechanism operates differently. Osteosarcoma, the most common bone malignancy in children and young adults, is typically treated with surgery followed by chemotherapy, but some tumour cells persist at the surgical site. Both curcumin and ginger extract inhibit the NF-kB signalling pathway, a molecular switch that cancer cells exploit to evade apoptosis and keep proliferating. In cell culture, the combined extract reduced osteosarcoma cell viability by roughly eleven-fold over eleven days, compared with uncoated implant controls.
In vivo testing used a rat distal femur model, where cylindrical implants were drilled into the bone and left for six weeks before the animals were euthanised and the femurs sectioned and stained. Three independent histological staining methods (Masson-Goldner trichrome, haematoxylin and eosin, and Sanderson’s rapid bone stain) all told the same story: the curcumin-ginger-zinc-hydroxyapatite combination produced approximately twice the new bone formation at the implant interface compared with uncoated controls. The drugs themselves release slowly, around 12% of the curcumin and 9% of the ginger extract over 28 days at physiological pH, with the two compounds appearing to enhance each other’s release when present together. That sustained, low-level delivery is probably more useful clinically than a single large dose, since the critical period for osseointegration and infection risk extends well into the first weeks after surgery.
Amit Bandyopadhyay, the Boeing Distinguished Professor at WSU and co-author on the paper, was direct about the scope of what the team is attempting. “There are many, many facets of this challenge,” he said. “This paper is focused on very big problems, and we’re telling the world a lot of little things you can do that may add significant benefit to the patient’s life, whether it’s a hip implant, knee implant, spinal implant, or shoulder implant. That’s really the holy grail of it.”
There are genuine caveats worth holding onto. Rat femur models are a standard early step, not a clinical outcome. The drug release fractions are modest, and it is not yet clear how the coating behaves under the cyclic mechanical loading that a hip or knee joint endures over years of use; some hydroxyapatite coatings are associated with increased revision risk over the long term, partly because of coating delamination. Human trials are some distance off.
Still, the multifunctional logic is compelling, perhaps because implant failure so often involves several problems at once rather than just one. A device that simultaneously promotes bone bonding, resists infection, and suppresses residual tumour cells at the surgical margin would address what are currently three separate clinical nightmares with a single coating that costs relatively little to add. Whether the zinc-curcumin-ginger combination holds up under the real demands of human joint loading is what the next phase of research will need to answer. Bose is optimistic that the compounds offer something beyond the implant application, too. “I’m very passionate about these natural medicinal compounds,” she said, “because I feel that they can be used so easily as preventative care in our everyday life.”
The deeper implication may be about where pharmaceutical chemistry is heading. Synthetic drug pipelines are expensive, slow, and prone to toxicity surprises; the appeal of drawing on compounds with millennia of human use behind them, and reasonably well-understood safety profiles, is obvious. Whether turmeric and ginger can do at the nanogram scale inside a bone implant what they appear to do in a curry bowl is a genuinely interesting question, and the early answer from Washington State suggests they can do quite a lot.
DOI: 10.1111/jace.70532
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.