A new experimental drug might finally offer hope for the millions of Americans trapped in a devastating cycle where trauma, chronic pain, and alcohol addiction feed off each other in an endless spiral of suffering.
Researchers at Florida Atlantic University have discovered that PPL-138, an opioid partial agonist, can simultaneously tackle three conditions that frequently appear together but have never been effectively treated as a unified problem. The findings, published in the British Journal of Pharmacology, represent a potential shift away from the current patchwork approach of multiple medications with limited success rates.
The numbers paint a stark picture of need. About 12 million American adults live with PTSD, but the real challenge emerges when you consider the overlap: 63% of veterans with PTSD also battle alcohol use disorder or chronic pain. When these conditions converge, they create a treatment nightmare where existing therapies often fall short or produce serious side effects.
Targeting the Anxious Brain
What makes PPL-138 particularly intriguing is its selectivity. In laboratory studies using rats exposed to prolonged stress, the drug didn’t work like a blanket sedative. Instead, it specifically helped animals that developed anxiety-like behaviors following trauma, leaving resilient animals largely unaffected.
“Our results show that PPL-138 not only reduces trauma-related anxiety and pain, but also selectively curbs alcohol use in rats most vulnerable to stress-induced drinking,” said Andrea Cippitelli, the study’s lead author and assistant professor at FAU’s Schmidt College of Medicine.
This precision targeting could address a major frustration in current PTSD treatment, where medications often help some patients while proving ineffective or harmful for others. The drug appears to identify and treat the specific brain pathways involved in trauma-related drinking, rather than simply suppressing alcohol consumption across the board.
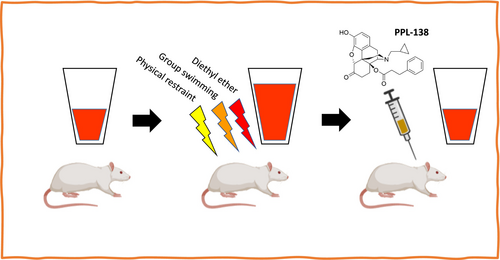
The research team divided rats into different groups, exposing some to chronic traumatic stress while keeping others as controls. Those that developed PTSD-like symptoms showed significant improvements in anxiety, pain responses, and alcohol consumption when treated with PPL-138. Crucially, the drug didn’t affect movement or cause sedation, suggesting its effects were genuinely therapeutic rather than simply suppressive.
Gender Differences Emerge
Perhaps most revealing were the sex differences the researchers uncovered. Female rats showed reduced alcohol intake when anxious, even without escalated drinking patterns. Male rats, meanwhile, were twice as likely as females to increase alcohol consumption following trauma, but only anxious males responded to the treatment.
“This mirrors well-documented patterns in humans, where women are more prone to anxiety-related disorders like PTSD and often use alcohol to cope with emotional distress, whereas men typically engage in heavier, more generalized drinking,” Cippitelli explained.
These findings could inform more personalized treatment approaches, acknowledging that trauma manifests differently across genders and may require tailored therapeutic strategies.
The research builds on decades of frustration within the medical community over the lack of effective treatments for co-occurring PTSD and substance abuse. Currently, no approved medications effectively treat both conditions simultaneously, forcing clinicians to prescribe multiple drugs that may interact poorly or produce competing side effects.
PPL-138 works by targeting specific opioid receptors in the brain, but unlike traditional opioids, it acts as a partial agonist. This means it provides enough activation to produce therapeutic effects while maintaining a ceiling that reduces the risk of overdose or severe side effects. The approach represents a middle ground between the powerful but dangerous full opioid agonists and the complete receptor blockers that can be too restrictive.
Phoenix PharmaLabs, which owns the intellectual property for PPL-138, is currently advancing the compound through clinical trials. The transition from animal studies to human trials will be crucial, as laboratory findings don’t always translate directly to clinical success.
The research team emphasizes that their work represents just the beginning of what could be a new approach to treating trauma-related conditions. The study was supported by the U.S. Office of the Assistant Secretary of Defense for Health Affairs, reflecting the military’s particular interest in finding better treatments for service members and veterans.
For the millions of Americans currently struggling with the interconnected challenges of trauma, pain, and addiction, PPL-138 offers something that has been frustratingly elusive: the possibility of addressing their conditions not as separate problems requiring separate solutions, but as aspects of a unified syndrome that might respond to unified treatment.
Whether this laboratory promise will translate into real-world relief remains to be seen, but the precision and selectivity demonstrated in these initial studies suggest that researchers may finally be approaching trauma-related disorders with the sophistication they demand.
British Journal of Pharmacology: 10.1111/bph.70151
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.