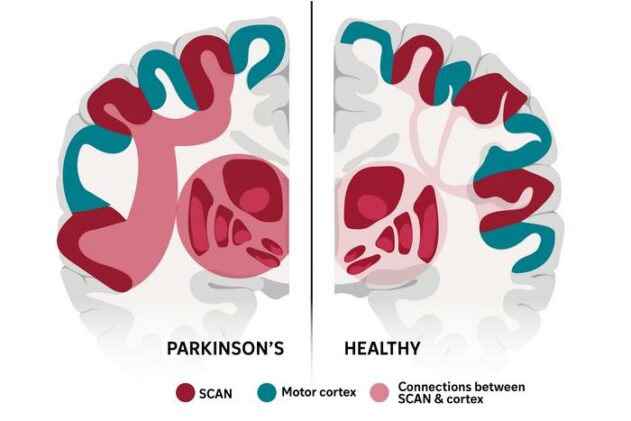
The brain has a secret. Threaded through the motor cortex, the strip of grey matter that controls movement, lies a network that nobody properly recognised until 2023. It alternates with the regions controlling your hands, feet and mouth, like piano keys interspersed among the white notes. This network, called SCAN, doesn’t just control individual body parts. It coordinates thinking with action, links arousal to movement, and ties organ function to behaviour.
And it might explain Parkinson’s disease.
More than 10 million people worldwide live with Parkinson’s, experiencing tremors, stiffness, and difficulty moving. But the disease has always been puzzling, really. It doesn’t just affect movement, it disrupts sleep, cognition, digestion, even motivation. That’s quite a range for something supposedly about motor control. For decades, neurologists focused on the basal ganglia, deep brain structures that help coordinate muscle movements. The substantia nigra loses its dopamine-producing cells, the circuit misfires, movements become difficult. Simple enough.
Except it wasn’t simple at all.
A massive study published this week in Nature suggests Parkinson’s isn’t fundamentally a movement disorder. It’s a SCAN disorder. Researchers in China and the US examined brain scans from 863 people, patients with Parkinson’s, people receiving various treatments, and healthy controls, and found something consistent across all of them. In Parkinson’s, the SCAN becomes hyperconnected to key subcortical regions. The wiring goes haywire, essentially. And when treatments work—whether deep brain stimulation, magnetic stimulation, focused ultrasound or medication—they calm that hyperconnectivity.
“This work demonstrates that Parkinson’s is a SCAN disorder,” says Nico Dosenbach at Washington University School of Medicine in St Louis, who co-authored the study. His team first described the SCAN network in 2023, revealing these interposed regions that had been hiding in plain sight. “The data strongly suggest that if you target the SCAN in a personalized, precise manner you can treat Parkinson’s more successfully than was previously possible.”
The researchers, led by China’s Changping Laboratory, weren’t just looking at scans. They tracked patients through multiple treatments over time. Fourteen people with Parkinson’s underwent deep brain stimulation surgery, receiving implanted electrodes in a region called the subthalamic nucleus. The team scanned them before surgery, then at one, three, six and 12 months afterward. Motor symptoms improved, as expected. But something else happened, too. The abnormal hyperconnectivity between SCAN and the subcortex decreased. The more it decreased, the better patients felt.
It wasn’t unique to one treatment. The researchers tested transcranial magnetic stimulation—magnetic pulses delivered through a coil placed on the scalp—in 36 patients. Half received stimulation targeted at SCAN regions, half at traditional motor areas. Both groups improved. But the SCAN group showed a 56 per cent response rate compared to 22 per cent in the other group. More than double.
Even levodopa, the standard Parkinson’s medication, reduced SCAN hyperconnectivity when it alleviated symptoms. Four different therapies, one consistent pattern.
Hesheng Liu, the study’s senior author, has spent years examining how brain networks go wrong in disease. “For decades, Parkinson’s has been primarily associated with motor deficits and the basal ganglia,” he says. But that framework couldn’t explain the cognitive symptoms, the autonomic problems, the sleep disturbances. The SCAN, though, coordinates action with thinking. It links your body’s internal state—arousal, organ function, physiological readiness—with voluntary movement and behavioural goals.
“Our work shows that the disease is rooted in a much broader network dysfunction,” Liu says. “The SCAN is hyperconnected to key regions associated with Parkinson’s disease, and this abnormal wiring disrupts not only movement but also related cognitive and bodily functions.”
Perhaps more interesting is what this means for treatment. Deep brain stimulation works, certainly. But it requires brain surgery, costs enormous amounts, and remains inaccessible to most patients. Only a small fraction of people with Parkinson’s are suitable candidates. Non-invasive approaches—magnetic stimulation, focused ultrasound from outside the skull—could reach far more people, especially earlier in the disease.
“With non-invasive treatments, we could start treating with neuromodulation much earlier than is currently done with DBS,” Dosenbach says. His team is planning trials using electrode strips placed on the scalp over SCAN regions to treat walking problems in Parkinson’s. They’re also investigating low-intensity focused ultrasound, which uses sound waves to modulate brain activity without breaking the skin.
The focused ultrasound results were intriguing. Ten patients with tremor-dominant Parkinson’s received the treatment, which uses sound waves to create a tiny lesion in the thalamus. The researchers calculated each patient’s optimal target based on their individual SCAN connectivity patterns. The closer the actual treatment site was to that personalised target, the better the outcome. Miss the sweet spot, and results suffered.
That precision might be the key, actually. The brain isn’t uniform. Your SCAN isn’t quite like mine. A treatment that works brilliantly for one person might barely help another if it’s hitting the wrong spot. The study showed that with careful mapping of each person’s unique brain networks—something that’s becoming increasingly feasible with modern scanning—targeting could become far more accurate.
There’s fire in this, clearly. Dosenbach has a financial interest in Turing Medical, a startup developing targeting software and brain stimulation systems. Liu is chief scientist of Neural Galaxy. That’s worth noting. But the findings come from 863 people across multiple sites, using different treatments and technologies. The hyperconnectivity pattern was consistent. When treatments reduced it, patients improved.
What happens next? Dosenbach suggests they need to understand whether different parts of SCAN affect different symptoms. The network isn’t monolithic—it has nodes, subregions, connections that might play distinct roles. Stimulating one area might help with movement, another with cognition. That sort of refinement takes time and careful research. But the framework is there now: Parkinson’s as a network disorder, SCAN as the central player, and personalised targeting as the way forward.
Roughly a century ago, researchers thought Parkinson’s was purely about muscle rigidity. Then came the dopamine discovery, the basal ganglia focus, increasingly sophisticated models of motor circuits. Each advance revealed new complexity. This SCAN finding doesn’t replace that work—the substantia nigra still matters, dopamine is still crucial, the subthalamic nucleus remains a key target. But it reframes everything within a broader network that explains why a disease about movement also affects thinking, motivation, sleep and organ function.
It’s the sort of reconceptualisation that changes treatment paths. And for the 10 million people worldwide navigating Parkinson’s symptoms, that might matter quite a bit.
Study link: https://www.nature.com/articles/s41586-025-10059-1
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.