Scientists have discovered human pegivirus—a relatively obscure virus from the same family as hepatitis C—in the brains of 50% of Parkinson’s disease patients examined, while finding none in healthy control brains.
The unexpected finding suggests this persistent virus may play a previously unrecognized role in the neurodegenerative disease affecting over 10 million people worldwide.
Researchers used an advanced viral detection system called ViroFind to scan brain tissue from 10 Parkinson’s patients and 14 age-matched controls. The technique can identify every virus known to infect humans, revealing that human pegivirus (HPgV) appeared exclusively in Parkinson’s brains—a statistically significant difference that raises questions about viral triggers in neurodegeneration.
Genetic Variations Shape Viral Response
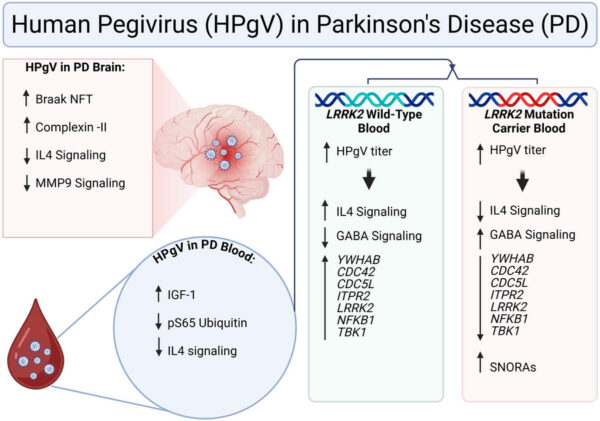
The research revealed striking differences in how patients respond to pegivirus infection based on their genetic makeup. Those carrying mutations in the LRRK2 gene—a known Parkinson’s risk factor—showed completely opposite immune responses to the virus compared to patients without the mutation.
When viral levels increased, patients with normal genetics showed enhanced immune signaling, while those with LRRK2 mutations experienced suppressed immune responses. This genetic-dependent pattern affected a network of 157 genes centered around YWHAB, a protein that helps regulate cellular functions critical for brain health.
The team analyzed brain tissue from three regions: the amygdala, posterior putamen, and superior frontal cortex. They confirmed viral presence using both genetic sequencing and antibody staining, which revealed pegivirus proteins in brain cells called oligodendrocytes.
Immune System Disruption
Patients with pegivirus in their brains showed more advanced disease pathology, including higher levels of tau protein tangles—a hallmark of neurodegeneration. They also had elevated levels of complexin-2, a protein involved in neurotransmitter release, suggesting altered brain communication.
Blood analysis revealed additional immune disruptions in pegivirus-positive patients:
- Higher IGF-1 levels: Suggesting metabolic changes
- Lower pS65-ubiquitin: Indicating disrupted cellular cleanup processes
- Altered IL-4 signaling: Affecting anti-inflammatory responses
- Persistent viral presence: Detected over years in longitudinal studies
Viral Persistence and Replication
Human pegivirus belongs to the flavivirus family, which includes hepatitis C and West Nile virus. Unlike many viruses that establish dormant infections, pegivirus appears to actively replicate in brain tissue. The virus typically causes no symptoms and can persist in blood for years or decades in 1-5% of the population.
The virus’s presence in brain tissue while being absent from blood samples in these patients suggests specific factors may facilitate its entry into the nervous system. Blood-brain barrier dysfunction or neuroinflammatory changes associated with Parkinson’s could create conditions allowing viral invasion.
Longitudinal analysis of blood samples from the Parkinson’s Progression Marker Initiative showed that viral infections could persist for over two years, with some patients eventually clearing the virus while others maintained persistent infections regardless of disease status.
Implications for Treatment
The discovery adds to growing evidence that viral infections may serve as environmental triggers for Parkinson’s disease. Historical examples include the 1918 encephalitis lethargica epidemic, after which some survivors developed Parkinson’s-like symptoms years later.
More recently, infections with West Nile virus, St. Louis encephalitis virus, and Japanese encephalitis B virus have been associated with Parkinson’s-like movement disorders. The current findings suggest that even seemingly harmless persistent viruses might contribute to neurodegeneration under certain conditions.
The research team emphasized that their work demonstrates association rather than causation. However, the consistent patterns across brain regions and the genetic-dependent immune responses support the hypothesis that viral infections interact with host genetics to influence disease progression.
Future studies will need to determine whether pegivirus infection occurs before or after Parkinson’s symptoms begin, and whether targeting viral infections or associated immune pathways could provide therapeutic benefits. The findings underscore the complex interplay between genetics, immunity, and environmental factors in neurodegenerative diseases.
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.