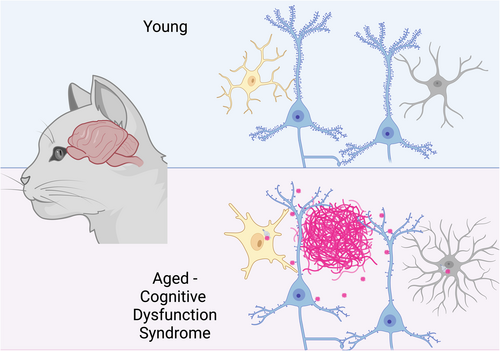
Older cats with dementia develop brain changes that closely match those seen in people with Alzheimer’s disease, according to new research from the University of Edinburgh. The study, published August 11, 2025, in the European Journal of Neuroscience, reveals that cats naturally accumulate toxic amyloid-beta protein in the brain, offering a valuable new model for studying the human condition and testing treatments.
Amyloid-Beta and the Aging Feline Brain
Scientists examined the brains of 25 cats of different ages after death, including animals with signs of feline cognitive dysfunction syndrome (CDS), often called feline dementia. Using high-resolution confocal microscopy, the team found amyloid-beta deposits within synapses, the tiny communication points between brain cells, in both aged cats and those with dementia. Synaptic loss is a strong predictor of memory decline in human Alzheimer’s disease.
The research also uncovered a surge of activity in two types of support cells: microglia and astrocytes. These cells were observed engulfing the damaged synapses in a process known as synaptic pruning. While pruning is essential during brain development, excessive pruning later in life can accelerate cognitive decline.
“Dementia is a devastating disease, whether it affects humans, cats, or dogs,” said Dr Robert McGeachan, lead author from the University of Edinburgh’s Royal (Dick) School of Veterinary Studies. “Because cats naturally develop these brain changes, they may offer a more accurate model of the disease than traditional laboratory animals, ultimately benefiting both species and their caregivers.”
Shared Symptoms, Shared Science
Many older cats with dementia display behaviors reminiscent of human Alzheimer’s symptoms, including:
- Increased vocalization, often at night
- Disorientation and confusion
- Altered sleep–wake cycles
- Changes in social interaction
Professor Danièlle Gunn-Moore, senior author and Personal Chair of Feline Medicine at the Royal (Dick) School of Veterinary Studies, noted that the similarities in brain pathology make feline dementia “the perfect natural model” for Alzheimer’s research. She added that understanding and treating the condition in cats could ultimately improve life for both pets and people.
Why Cats May Outshine Rodents in Alzheimer’s Research
Most Alzheimer’s research to date has relied on genetically modified mice, which do not naturally develop dementia. The Edinburgh study suggests that cats could serve as a more realistic, non-engineered model, providing insight into disease progression and response to potential treatments in a naturally aging brain.
Researchers found that while aged cats and those with dementia had similar overall amyloid-beta burdens, only in the dementia group did the protein strongly correlate with increased synapse loss. This mirrors findings in human studies, where amyloid presence alone does not guarantee disease severity. It is the combination of amyloid buildup and glial cell activity that appears to drive neurodegeneration.
Looking Ahead
The authors acknowledge limitations, including the small sample size and challenges in detecting subtle cognitive changes in aged control cats. They also call for future studies using higher-resolution imaging to confirm the extent of amyloid-beta within synapses. Despite these caveats, the work underscores the potential of feline dementia research to inform both veterinary and human medicine.
The study was funded by Alzheimer’s Research UK, the UK Dementia Research Institute, and the Wellcome Trust.
Journal Reference
European Journal of Neuroscience, “Amyloid-Beta Pathology Increases Synaptic Engulfment by Glia in Feline Cognitive Dysfunction Syndrome: A Naturally Occurring Model of Alzheimer’s Disease,” DOI: 10.1111/ejn.70180
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.