A simple headband that shines laser light into the forehead could revolutionize how doctors monitor blood flow in the brain, offering a low-cost alternative to expensive imaging machines. The device, developed by researchers at USC and Caltech, solves a problem that has vexed scientists for years: how to measure what is happening inside the brain without the scalp getting in the way.
The technology relies on speckle contrast optical spectroscopy, a technique that sounds more complicated than it is. Tiny blood cells moving through vessels scatter laser light in predictable patterns. By analyzing how those patterns blur and shift, the device can calculate how fast blood is flowing. The challenge has always been distinguishing between blood vessels in the scalp, which sits just beneath the skin, and those deeper in the brain tissue itself.
A Creative Test Using Temporary Blockage
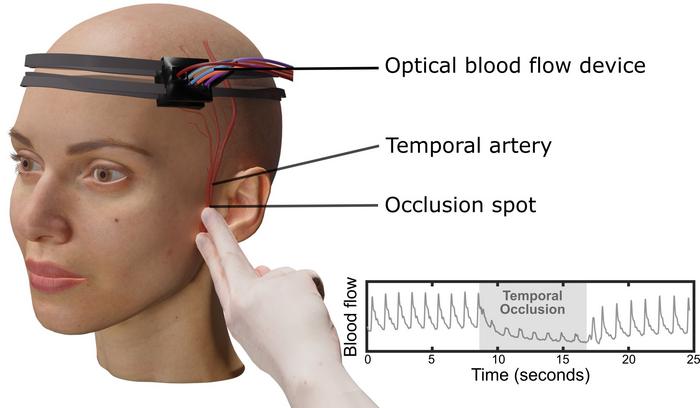
To prove their device was actually seeing brain blood flow rather than just scalp circulation, the research team took an unconventional approach. They temporarily blocked blood flow to the scalp by gently pressing on the superficial temporal artery, a vessel near the temple that feeds the front portion of the scalp. Twenty volunteers participated in the experiment, which involved a few seconds of pressure followed by measurements from seven detectors arranged at increasing distances from the light source.
The results were revealing. When blood flow to the scalp stopped, signals from detectors positioned close to the skin dropped dramatically. But detectors placed farther away, at least 2.3 centimeters from the laser source, continued picking up strong signals. Those distant readings, the team concluded, were coming from blood vessels in the brain.
“For the first time in humans, this experimental evidence shows that a laser speckle optical device can probe beyond the scalp layers to access cerebral signals.”
The finding marks a departure from previous research, which relied on statistical simulations to estimate which signals originated where. By creating a real-world change that affected only the scalp, the researchers could directly test their device’s ability to peer deeper.
From Animal Studies to Human Applications
Speckle contrast optical spectroscopy has been used in animal research for years, but adapting it for clinical use in humans required solving the scalp problem. The brain’s blood supply is critical for diagnosing and responding to conditions like stroke, traumatic brain injury, and vascular dementia. Current imaging methods such as MRI and CT scans are effective but expensive and not widely available, particularly in emergency or resource-limited settings.
Charles Liu, director of the USC Neurorestoration Center and co-senior author of the study, emphasized the device’s simplicity. It uses an affordable high-resolution camera to capture images of scattered laser light. No bulky machinery, no radioactive tracers, no claustrophobic tubes.
“We’ve established a safe, simple, and repeatable experimental framework that other researchers can use to validate their own noninvasive optical systems.”
The headband configuration makes the technology particularly practical. Worn across the forehead, it houses both the light source and the array of detectors. The closer detectors capture shallow signals from the scalp, while those positioned farther away pick up deeper, broader data that includes brain blood flow. By identifying which signals are superficial, the device can isolate the deeper signals corresponding to circulation in the brain itself.
Individual variation poses another challenge. Some people have thicker scalp or skull layers than others, which affects how light penetrates and scatters. The research team is working to refine the technology so it can be used across diverse patient populations without requiring extensive calibration for each person.
The study, published in APL Bioengineering and funded by the National Institutes of Health, the Alfred Mann Foundation, and the USC Neurorestoration Center, represents an important step toward clinical deployment. Because all testing has been conducted with human participants rather than animal models, the path from laboratory to bedside could be relatively short. Some collaborators are already using the technique to help diagnose stroke and traumatic brain injury in clinical settings.
Next steps include improving image resolution and data quality, as well as adding a sensor that allows the device to be placed directly on the skin for better contact and more consistent readings. The team also plans to expand testing with patients in hospitals and clinics, building on the foundation established by this validation study.
APL Bioengineering: 10.1063/5.0263953
ScienceBlog.com has no paywalls, no sponsored content, and no agenda beyond getting the science right. Every story here is written to inform, not to impress an advertiser or push a point of view.
Good science journalism takes time — reading the papers, checking the claims, finding researchers who can put findings in context. We do that work because we think it matters.
If you find this site useful, consider supporting it with a donation. Even a few dollars a month helps keep the coverage independent and free for everyone.